
Breast Cancer Awareness Month is as good a time as any to brush up on your knowledge, mama. Check out our expert advice on early detection, risk factors, and where you can get screened.
Breast cancer is the top cancer in women both in the developed and developing world. As October is Breast Cancer Awareness month, and with new research constantly emerging, we thought it was a good time to brush up on our knowledge, so we spoke with Dr. June Tan Sheren at International Medical Clinic (IMC) to get some facts.
In Europe, the United Kingdom, Australia and the United States, about 1 in 8 women (12%) will develop invasive breast cancer during their lifetime. The American Cancer Society estimates that in 2016, about 246,000 new cases of invasive breast cancer will be diagnosed in the US alone. The chance that a woman will die from breast cancer is about 1 in 36 (about 3%). Death rates in developed countries have been dropping in recent years and this is believed to be the result of finding breast cancer earlier through screening and increased awareness, as well as better treatments. Figures from Australia show that between 1983–1987 and 2008–2012, 5-year relative survival from breast cancer improved from 72% to 90%.

What are the symptoms of breast cancer?
Different people have different symptoms of breast cancer, and some people do not have any signs or symptoms at all. A woman may find out she has breast cancer only after a routine mammogram.
It is important to know the normal look and feel of your breasts. Things you should look out for include:
- a new lump or lumpiness in your breasts, especially if it is in only one breast
- a change in the size and shape of your breast
- a change to the nipple such as crusting, an ulcer, redness or the nipple pulled in
- a change in the skin of your breast such as redness, dimpling or puckered skin
- a pain that does not go away
Most breast changes will not be due to breast cancer but you should get them checked. If you notice a change in the look or feel of your breasts, even if your screening mammogram was normal, see your GP without delay. The symptoms of breast cancer depend on where the tumour is in the breast, the size of the tumour and how quickly it is growing.

What are the risk factors for breast cancer?
Studies have shown that a woman’s risk for breast cancer is due to a combination of factors. The main factors that influence risk are simply being a woman and getting older. Most breast cancers are found in women 50 years of age and above.
Risk factors include
- Genetic mutations. Inherited changes (mutations) to certain genes, such as BRCA1 and BRCA2, increase a woman’s risk of breast and ovarian cancer.
- Longer exposure to your body’s hormones, such as women who start their periods before age 12, or start menopause after age 55, raises the risk for breast cancer by a small amount.
- Late or no pregnancy. Having the first pregnancy after age 30 or never having a full-term pregnancy can raise breast cancer risk.
- Not being physically active.
- Being overweight or obese.
- Drinking alcohol. Studies show that a woman’s risk for breast cancer increases with the more alcohol she drinks.
- Family history of breast cancer. A woman’s risk for breast cancer is higher if she has a mother, sister, or daughter (first-degree relative) or multiple family members on either her mother’s or father’s side of the family who have had breast cancer. Having a first-degree male relative with breast cancer also raises a woman’s risk.
- Using combination hormone therapy such as HRT in the menopause, or combination oral contraceptives.
- Personal history of breast cancer. Women who have had breast cancer are more likely to get breast cancer a second time.
- Previous treatment using radiation therapy to the chest or breasts (like for treatment of Hodgkin’s lymphoma).

How do I lower my risk of breast cancer?
Keep a healthy weight and exercise regularly at least 4 hours a week. Don’t drink alcohol, or limit alcoholic drinks to no more than 1 per day. If you are taking hormone replacement therapy or combined oral contraceptives, ask your doctor about the risks and find out if it is right for you. Breastfeeding is associated with a lower risk of breast cancer.
If you have a family history of breast cancer or inherited changes in your BRCA1 and BRCA2 genes, it is important to talk to your doctor about more ways to lower your risk and screening for early cancer detection.
Staying healthy throughout your life will lower your risk of developing cancer, and improve your chances of surviving cancer if it occurs.
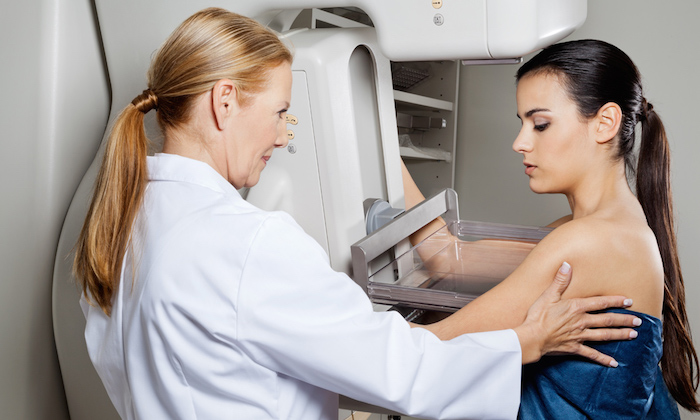
How do I screen for breast cancer?
Mammography is widely accepted as the best method to detect breast cancer early, when it is easier to treat and before it is big enough to feel or cause symptoms. Having regular mammograms lowers the risk of dying from breast cancer by up to 35% in women between the ages of 50 and 69. Finding any abnormalities early ensures that women have all treatment options available to them. The earlier breast cancer is found, the better the chance of surviving it. Leading health organizations around the world recommend that women who are 50 to 74 years old and are at average risk for breast cancer get a mammogram every two years. Women who are 40 to 49 years old should talk to their doctor about when to start and how often to get a mammogram.
According to the Breast Cancer Foundation, subsidised mammography is available through the Health Promotion Board for Singaporean women and Permanent Residents aged 40 and above who have not had a mammogram in the last 12 months. The cost is $50 and mammograms are available at several polyclinics across the island. To make an appointment call 1800 333 3030, or email [email protected] for more information.
If you’re not Singaporean or PR, you can of course still get a mammogram with a referral from your GP.
The majority of women who have a screening mammogram will get a normal result. Women should still continue to know the look and feel of their breasts between screening mammograms, and report any changes to their GP.
Some women will be called back for more tests because the mammogram showed an abnormality. For most of these women, subsequent tests are normal and breast cancer is not found. Women diagnosed with breast cancer following a screening mammogram are less likely to have a mastectomy (have their breast removed). Depending on a number of factors and the stage of the cancer, other treatment options can include chemotherapy, radiotherapy and hormonal therapies.
![]()
As a woman well entering into her forties, as a wife and a mother, and as a family physician with an active practice in preventive care, breast cancer is a topic that is close to my heart. My key message to you is live a healthy lifestyle, know your body, and see your doctor for regular screening – early detection saves lives.
References:
Cancer Australia
Centres for Disease Control and Prevention
American Cancer Society
European Society for Medical Oncology
International Medical Clinic (IMC)
Camden Medical Centre, 1 Orchard Boulevard, #14-06, Singapore 248649, Tel: (+65) 6733 4440
293 Holland Road, #02-04 Jelita Shopping Centre, Singapore 278628, Tel: (+65) 6465 4440, www.imc-healthcare.com






 View All
View All





 View All
View All









 View All
View All







