
 Post Category - ParentingParenting - Post Category - BabyBaby - Post Category - Toddler & PreschoolerToddler & Preschooler - Post Category - Older KidsOlder Kids
Post Category - ParentingParenting - Post Category - BabyBaby - Post Category - Toddler & PreschoolerToddler & Preschooler - Post Category - Older KidsOlder KidsWe hear from two mothers whose kids got COVID-19. Plus save this doctor’s step-by-step guide of what to do if you suspect your child has the virus
It’s every parent’s nightmare – you get a call that your child has been exposed to COVID-19. What should you do? One mother and baby had to be hospitalized while another mom could isolate at home with her toddler – both share their tips. If you suspect your child has COVID-19 or they test positive, don’t panic (easier said, we know!) From MOH statistics, children to date in Singapore have had very mild COVID-19 infections and many are asymptomatic. That said, you’ll need to know the proper steps to take – so we get a paediatrician’s advice on what to do plus red flag signs to watch for.
Jump to:
Personal story: Both kids got COVID-19. My baby was hospitalized
Personal story: We isolated at home after my toddler and I got COVID-19
Step-by-step guide if you suspect your child has COVID-19
Should you go to A&E or not? Red flags to watch for
Can children recover at home or must they be hospitalised?
‘Both my kids got COVID. My toddler isolated at home, my baby was hospitalized’
Lilian, mother to a 3.5-year-old son and a 5-month-old baby found out her eldest was COVID-19 positive:
When I saw those two lines appear on my child’s Antigen Test, my heart sank. Pangs of guilt washed over me. Where did my child catch it? Both parents were vaccinated and we didn’t go out much. COVID-19 still had a certain amount of social stigma attached to it, even as Singapore is transitioning to treating it as an endemic disease. Thanks to our strong support system, I was able to snap out of that guilt phase quickly. After all, I had two sick children and I was pretty sure I was getting COVID-19 from them (Spoiler Alert, I did get it). My child’s school was warm and supportive, as were my friends and family.

How did you find out your child had COVID-19?
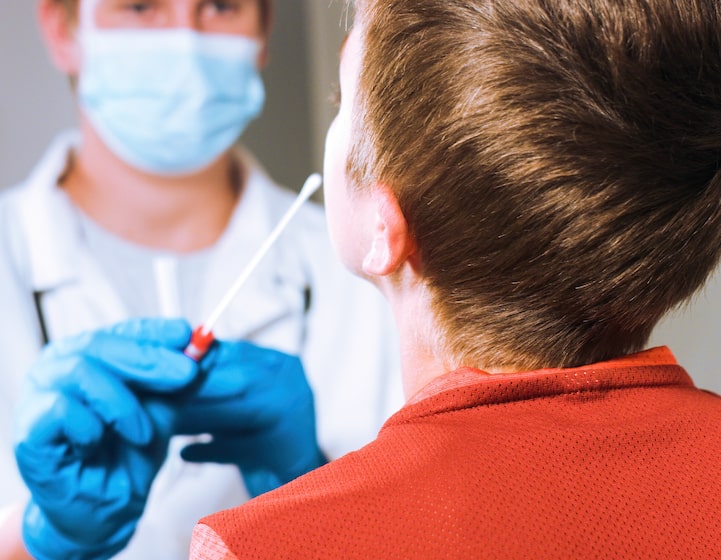
My 3.5-year-old son woke up one day with a fever. We informed his daycare immediately – this allowed them to start contact-tracing (testing his classmates and staff) and disinfecting the school. Luckily, no one else tested positive in the school. We did an Antigen test on him, which was positive. We then brought him to a SASH clinic for a PCR swab and received the positive results later that day. For my 5-month-old infant, we noticed he was feeling feverish and getting very fussy. We did an Antigen test on him (very gently) and got positive results. However, the SASH clinic we called told us to go down to KKH to get a PCR swab due to the young age of our infant. We did that and got a positive result the next day.
The following days, we received calls from contact tracers, MOH officers and also a visit from MOH to make sure that my eldest was at home during his isolation order. Our 3.5-year-old was meant to get sent to a hospital for evaluation to assess that he was suitable for home recovery, but due to a system backlog, we did not get that notification until day 6 of his home recovery period. We gave him some paracetamol to bring his fever down, and that was about it. Lots and lots of movies, cuddle time and ice blended milo (my child’s favourite drink!). After day 6, he was fully recovered, so we turned down the hospital assessment.
For our baby, the events were a bit more harrowing. Following his positive COVID-19 test, we weren’t sure how long it would take for MOH to arrange for us to be sent to the hospital, since we were not eligible for home recovery. After a few hours of seeing the condition of our infant worsen (not breastfeeding, increased fussiness, repeated coughing and looking breathless), we took the advice of MOH and Certis officers we had talked to and called 995 to be transported to KKH immediately.
My infant and I (breastfeeding mother) were warded in a pediatric isolation room. My infant was closely monitored and given medication to help with his fever, congestion and runny stools. After 6 days, we were able to be discharged for home recovery.
How did you find the hospitalization?
My husband and I had quarantined in a hotel last year with our toddler when we moved to Singapore, so I thought I could handle a hospital stay with an infant. Nope, I was wrong. This was way tougher! The first 24 hours were emotionally and physically draining. My child wailed through the night, and the doctors and nurses came in often to check on our vitals. I barely ate, drank or slept. I developed the textbook symptoms of COVID-19: high fever, cough, congestion, sore throat, headache and anosmia. All through the day and night, I could hear other children crying in the other isolation beds. Since I was a caretaker, I didn’t have a hospital bed to recover in. Instead, I slept on the provided fold-out bed and breastfed on a plastic hospital chair. I didn’t know how I was going to make it through the stay!
After a very dark 12 hours, I reached out to my close friends and asked them to help me brainstorm coping techniques for my mental health and their support really helped me. The nurses helped me manage my COVID-19 symptoms with appropriate medication. I developed a routine and something to look forward to, like journalling, and opening/ closing the shades for every naptime, and playing certain types of music during periods of the day. Occasionally, I sent myself a treat using GrabFood. I used the baby carrier endlessly and sang to my infant for every nap. I chatted with my friends and updated them on our status every hour. I spoke to my husband and toddler multiple times a day. And when things got too overwhelming (and they did, many times), I put my infant down in a safe place, sat in the ensuite bathroom and bawled. Hour by hour, we slowly made it over the finishing line- the doctors got our early discharge approved on the 6th day and we are now recovering at home.
What were their symptoms, if any?
My 3.5-year-old son had a fever for 3 days, followed by congestion, runny nose and eventually a bit of coughing. He was pretty much back to normal after about a week! Honestly, he had worse symptoms from the cold he caught last month. My baby had a fever for 3 days, with congestion, runny nose, coughing and runny/loose stools. He was also very fussy and couldn’t breastfeed more than a couple of minutes before crying. It’s been just over a week and he is almost back to his normal happy self too.
What was the advice for the rest of the household when you found out about the positive results?
Once our children had positive PCR results, the rest of the household was immediately on Health Risk Warning (HRW). We had to submit an Antigen Test on the first day, and made sure we had a negative ART for the next 6 days if we had to leave our home. We monitored our own temperature/oxygen levels daily.
Anything you wish you had known before or that you think may help others?
– Once your child has a positive Antigen test, you should take him/her in for a PCR swab as soon as possible. Use private transport and ask the driver to keep the windows down and air-con off. The isolation order/health risk warning only starts on the day of your swab, so go as soon as possible.
– Make sure you call up the SASH clinic before heading down. Some clinics don’t swab children or infants, and some prefer you come in at certain times of the day.
– Once you have taken your child for the PCR swab, make sure you keep your phone near you as you’ll be getting a lot of important calls and messages.
– If your child’s PCR test is positive, you CANNOT take private transport (taxi, grab etc). You will have to wait for MOH’s transportation services, or in case of an emergency, an ambulance can transport you to the hospital.
– If your child goes to daycare or school, inform the school immediately so they are aware and can kick start protocols on their end. This will help with limiting transmission at school.
– For moms with young infants below 1, if they do test positive for COVID-19, you will have to be hospitalized. It is not optional. You don’t have to call anyone- MOH will get in touch with you to transport you and your infant to a care facility. Start tracking your infant’s input and output (how much they are eating and how many wet diapers and so on), as the nurses will want that information once you are warded. I actually got a call from MOH within an hour of my infant’s positive PCR test, so I know they did take it very seriously. Don’t panic and don’t be afraid of going to the hospital. It will not be easy, but the wonderful nurses and doctors will take care of you and your infant. If you don’t have time to pack everything, don’t worry as you can get items delivered to the hospital later on. The average stay is 5-10 days, depending on your infant’s recovery.
‘When my son developed symptoms after being issued an HRWO, I knew he caught it’

Jumaiyah, mother to a 2.5-year-old toddler who contracted COVID-19:
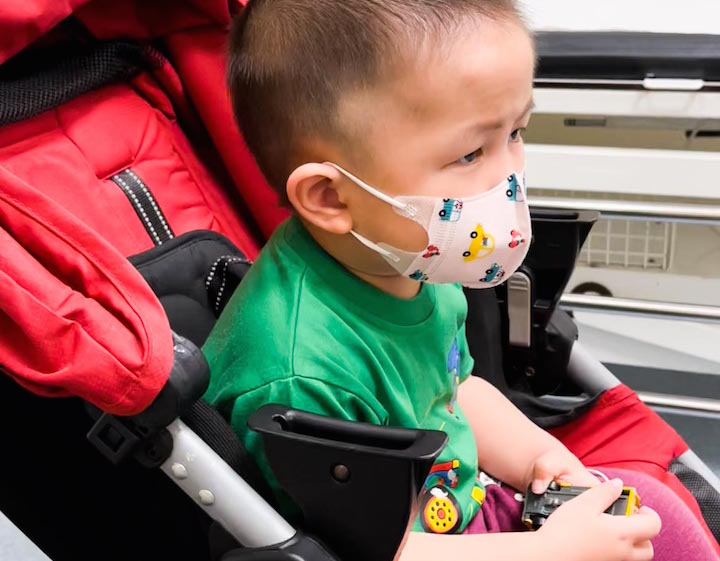
My son Muadz first received a notice from his pre-school stating that one of his schoolmates had contracted COVID-19. From there we picked him up from school as it was going to be shut immediately for 3 days (this is before the notice for the current measure to only close for 1 day). We then received the HRWO from MOH via SMS and stated isolating ourselves at home. We did the ART test for him on 17 October. Since it came out negative, we thought everything was fine and we’ll send him back to school when it opens 3 days later. Unfortunately, Muadz developed fever on the morning of 18th October and I already suspected that he had contracted the virus. We did the ART and true enough it came up positive, so we went to the SASH clinic to see the doctor for a PCR test for confirmation and also medication since Muadz had symptoms of fever, cough and flu and he was behaving a little out of sorts.
Muadz is only 2.5 years old. He is a playful bubbly boy that thrives on hugs and kisses. When he contracted COVID-19, I knew that he needed to be at the best of his mental wellbeing so that he can recover quickly, so I played with him and kept him company during the times that he wasn’t resting. And yes that involves hugs and kisses too. Doctor advised me to always have a face mask on, consistently sanitise and to always take precautions in order to not catch, but with the constant demands for hugs from the little one, it made it really hard for me to stay away from my son. And hence I caught the virus too, and tested positive 5 days later. I’m sure many parents of little children would empathise.
What were the symptoms if any?
Muadz’s symptoms were fever, cough and flu. I’m sure he felt some lethargy and body aches as this translated into crankiness and restlessness. But this didn’t last too long, he was well about 4 days later.
I think he fared way better than me with COVID-19. For me I had a persistent cough, an extreme headache, fever, and flu. On the first day of testing positive, I had chest pains that made it impossible for me to do anything else other than just lie down and rest. The chest pains went away after a day. I also lost my sense of taste and smell on day 4 of my isolation. It was really funny how I couldn’t smell my boy’s soiled diapers when he needed change! The most annoying symptom was the lethargy, which lasted more than a week after testing negative on ART. Though I tested negative on ART on day 6 of my isolation, some of the symptoms still remain until today.
Tell us about the events that unfolded after you found out about the positive result.
When Muadz developed a fever and tested positive on his ART, I was most concerned about his high fever, and needed medication for it. So what I did first was to call Muadz’s doctor to ask him if we could consult with him for Muadz’s fever medication. His clinic advised us that the protocol was to go to the nearest SASH clinic, and we should not consult with him.
At this point, we also knew that we will be needed more ART kits so we went with Muadz’s Birth Certificate (required for scanning) to collect ART test kits at the nearest vending machine.
When in consultation with the doctor at the SASH Clinic, he advised that it is very likely that Muadz will test positive on his PCR test seeing the events that led to him there, as well as seeing that he had symptoms on top of a positive ART test. The doctor gave us 2 options:
(1) To go to KKH immediately for PCR Swab and assessment or (2) For him to do the swab at the clinic and wait for PCR Results at home.
Here, a panicky mom’s instinct would be to go KKH immediately so that just in case the child tests positive, that we would already be in the hospital for any required treatment or procedures – I had wanted to do that too! But when I asked the doctor to explain further on what is to be expected for both options, I decided that it would be better for us to proceed with the swab test, and wait for the results at home.
Here are the reasons why we didn’t want to go to KKH immediately with a highly likely COVID-19 positive child.
- We didn’t have our own vehicle, and to take a taxi or even SHN Grab to go to KKH would be putting the respective drivers at risk, and we didn’t want to do that.
- We didn’t know what the current conditions at KKH were. If we had gone there immediately, we would have arrived without an appointment and been treated like a walk-in case. So, what if the wait time at the A&E at KKH was long? I wouldn’t want to be stuck at any waiting area with a child that has fever and is coughing due to COVID-19. It would be better for him to be swabbed at the SASH Clinic, to take the doctor’s medication then, and to rest in the comfort of our own home while waiting for whatever protocols from MOH that ensued. So that’s what we did.
After finding out Muadz’s positive result on the PCR test, we isolated at home and within the same day we were contacted by the Home Recovery Buddy who informed us that we could consult with a doctor via video call and if we needed, medicine could be sent to our home. A patient care team called and assessed Muadz’s symptoms. For ‘invisible’ symptoms like loss of taste and smell, or tummy ache, this would translate as a loss of appetite and just general crankiness when our kids feel discomfort. It is important to look out for these too!
The woman I spoke to on the phone then went ahead to talk about how Muadz needed to be assessed by KKH before he could be placed on HRP, and proceeded to schedule a pick up for us. For kids under 4, they may be sent to NUH or KKH for this. Since KKH was nearer our home, we insisted on KKH and thankfully there was a pick up slot for KKH available then. The earliest pick up was for 9am the next day. She also specifically mentioned to call 995 and ask for KKH immediately (without waiting for the next day pick up) should Muadz start exhibiting shortness of breath or if his fever at 39 degrees didn’t break that evening.
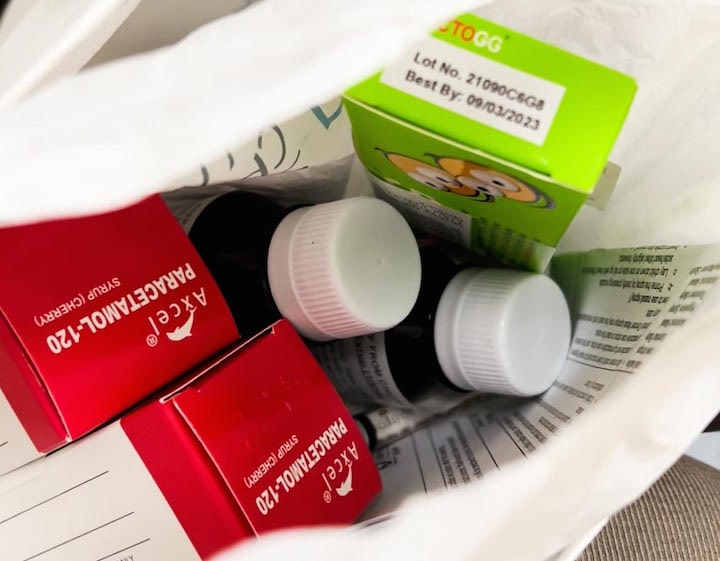
After our assessment at KKH, the doctor provided medication and included probiotics as part of his treatment. I also supplemented his recovery with Vitamin C. They checked on his breathing, and also his oxygen levels via the oximeter. When Muadz was ready to be discharged to recover at home, the rest of the family was advised to always wear a mask, to always wash hands and to isolate from COVID-19 patients to prevent the spread of the virus. This was pretty easy for us to do because at home, it’s just the three of us.
How is your son doing now? Any ongoing symptoms/issues?
He’s doing alright, fully recovered and back to his active self. We just went for a leisurely walk last weekend and he ran around for a good km or so, I could barely keep up. Throughout the whole ordeal, my husband did not catch the virus and tested negative on his daily ART.
Anything you wish you had known before or that you think may help others?
The most important item throughout this entire ordeal with COVID-19 should you ever need to face it, is your phone. You’ll be contacted constantly so be sure to keep it fully charged ALWAYS.
I wish I had known how sick I would be during the ordeal, and how long-lasting the symptoms of COVID-19 are, even for vaccinated individuals. It was not easy to feel lethargic, to constantly have a throbbing headache and not feeling like my best self for a whole 3 weeks. Some people still have yet to get their sense of smell and taste back even after months of testing positive. If I had known all of these, perhaps I would have done better with preventing myself from catching the virus when looking after Muadz. Also, maintaining a healthy immune system is important for combating the virus. So, if I had known all of these earlier, I would have probably included more vegetables, fruits and proteins in my diet, and exercise for a stronger heart.
Catching the virus is now a very high likelihood for most of us, so let’s be prepared for it by staying healthy and getting vaccinated.
Step-by-step guide if you suspect your child has COVID-19

If you suspect your child has COVID-19, what should you do? We get a step by step breakdown from Dr Lim Yang Chern, Consultant Paediatrician at Thomson Paediatric Centre (Jurong East Branch).
1. Confirm the diagnosis
2. Prepare your child (and yourself) for the swab
3. Treat your child if needed while awaiting advice from MOH
1. Confirming the diagnosis: You must bring your child for a confirmatory test. The ART test is not very sensitive and a negative ART may provide a false sense of security. If your child fits the testing criteria, a PCR test for COVID-19 must be done.
2. Prepare your child: This really helps alleviate much anxiety when parents have prepped the child prior to taking the test. Depending on the child, it can help to role-play a bit with a toy bear at home about what to expect during a swab test.
Prepare yourself: A swab, when done properly, will cause tearing and sometimes bleeding. This is because when there’s an upper respiratory tract infection, the tissues in the nose are naturally engorged and the blood vessels are often more friable and hence liable to bleed even on gentle contact. This can cause some contact bleeding – do not be alarmed. In fact, if the swab was not uncomfortable, chances are it was not done properly. The swab needs to rub against the nasal tissues to get a good sample and that in itself is not pleasant.
There are two main ways to perform the COVID-19 test – the oropharyngeal and mid-turbinate (OPMT) or “mouth and nose” test and the nasopharyngeal (NPA) test.
The OPMT test: is less uncomfortable as we only need to swab the back of the throat and the middle part of the nose.
The NPA test: is more uncomfortable as we need to swab all the way to the back of the nose for this.
If you have a child with special needs – a home rehearsal and plan will go a long way to making the process at the doctor’s office smooth and quick. I find this website useful. Many young children cannot co-operate with the OPMT/“mouth and nose” test as they cannot open their mouths long enough and sometimes bite down on the swab stick posing a risk of breakage of the stick. Hence, with all things considered, the best method to get a good sample for PCR in young children is still the NPA swab.
3. Treat your child if needed while awaiting advice from MOH
– Don’t panic and don’t worry. From MOH statistics, children to date in Singapore have had mild disease from primary COVID-19 infection.
– Treat your child as if they have the flu. Treat the fever when high/when your child is uncomfortable, hydrate your child well, get plenty of rest.
– After the initial positive test, MOH will contact you and advise your next steps. In general:
– Younger children will have a face-to-face assessment with a doctor, again this is arranged by MOH.
– Older children will have a teleconsultation assessment arranged. Medications will be provided as needed. Most cases do not need more than usual flu and fever medications.
– Infants (i.e. less than 1yr old) will usually be transported for admission for observation. One of the reasons for this is that children this age are more vulnerable in general and are unable to vocalize discomfort/pain accurately.
– Do not go to the A&E or call 995 unless it’s an emergency or you’ve been given explicit instructions to do so by MOH officials.
To go to A&E or not?
It is important to know when to call for help. It can take some time for MOH to arrange for transport. If your child is COVID-19 positive and is not showing any worrying symptoms, do not call 995 as your first port of call. If however your child has any red flag symptoms, consider calling 995 for help and they can transport your child in a safe manner to the nearest paediatric facility. These red flags also apply in general for any illness, not just COVID-19.
Some red flags include:
- Fever > 41 degrees Celsius
- Chest pain / difficulty breathing (especially if your child is rested and still panting for breath)
- Blue lips/tongue
- Any losses from vomiting/diarrhea with poor feeding
- Any persistent abdominal pain e.g. continuous for more than 30min
- Confusion e.g. cannot tell you time (day/night) or where they are or who you are
- Inability to stay awake i.e. drowsy
Can children recover at home if preferred or must they be hospitalised?
If your child is otherwise healthy and without chronic long-term disease, home recovery should be safe. Do not forget to take into account the other people at home. If home recovery puts other vulnerable people at home at risk of severe COVID-19 disease, then sometimes admission may be needed for the child.
Hospital beds are a limited resource and so it is a tenuous balance between resources and patient load that MOH with the partner hospitals need to maintain. Most children experience nothing more than the usual flu symptoms i.e. fever, runny nose, sore throat and cough. For these patients, home recovery is perfectly safe.
At every checkpoint, there are medical criteria to help risk-stratify your child – let your doctors make that assessment and guide your care. Part of the risk stratification includes past medical problems of the child, for example a child with chronic heart, lung or metabolic disease. In these cases, their primary physician should be able to provide advice on the risks of home recovery. If your child is deemed high risk – hospitalization will be advised to ensure the safety of the child.
Disclaimer: Information on home recovery and hospital admission is accurate at the time of publishing. Subject to changes by MOH as Singapore’s COVID-19 situation evolves.
For more information check out www.covid.gov.sg.






 View All
View All




 View All
View All









 View All
View All






