
Curious about the mastectomy vs lumpectomy dilemma, and other breast cancer treatment options in Singapore? A leading breast cancer surgeon (and mama) answers our questions
As Breast Cancer Awareness Month 2019 draws to a close, we wanted to continue our coverage with a closer look at breast cancer treatment options, including the perpetual dilemma that many women struggle with when diagnosed with breast cancer: mastectomy vs lumpectomy.
 Last year we heard from a molecular biologist about advances in preventing and treating breast cancer from the inside. This year we spoke to breast surgeon Dr. Jendana Chanyaputhipong of PanAsia Surgery Group to get more information on the pros and cons of mastectomy vs lumpectomy, along with some promising information on new cutting edge alternative treatments that are less invasive and reduce recovery time. An award-winning instructor at NUS and a mother to a young son, Dr. Jendana also completed a fellowship in the Breast Surgical Oncology sub-specialty, including the latest techniques in oncoplastic surgery, immediate or delayed reconstruction, and lipofilling as part of comprehensive treatment for breast cancer patients.
Last year we heard from a molecular biologist about advances in preventing and treating breast cancer from the inside. This year we spoke to breast surgeon Dr. Jendana Chanyaputhipong of PanAsia Surgery Group to get more information on the pros and cons of mastectomy vs lumpectomy, along with some promising information on new cutting edge alternative treatments that are less invasive and reduce recovery time. An award-winning instructor at NUS and a mother to a young son, Dr. Jendana also completed a fellowship in the Breast Surgical Oncology sub-specialty, including the latest techniques in oncoplastic surgery, immediate or delayed reconstruction, and lipofilling as part of comprehensive treatment for breast cancer patients.
Breast Cancer Treatment: Advances in Avoiding Chemo & Minimising Your Risk of Cancer
What is the difference between a lumpectomy and mastectomy? What are some typical situations in which each one might be recommended over the other?
A lumpectomy is the removal of the area of breast tissue that contains the abnormality, so what is removed is the tumour with a rim of normal-looking tissue that is referred to as the ‘margin’.
A mastectomy is the removal of the entire breast tissue, leaving just the skin above and the muscle below. There are different types of mastectomy. In simple mastectomy, part of the skin and the nipple-areolar complex is also removed. The patient is left with a scar across the chest. In nipple-sparing mastectomy, only the breast tissue is removed, leaving an intact skin envelope as well as the nipple-areolar complex. In skin-sparing mastectomy, the nipple-areolar complex is removed, leaving the skin envelope behind. The latter 2 types of mastectomy are usually performed followed by immediate reconstruction.
In patients with widespread disease, involving more than one area of the breast, mastectomy is usually recommended. In patients with localised disease, lumpectomy can be performed safely and with acceptable cosmetic outcome. However, it is important to remember that radiation therapy is required after lumpectomy, so if anyone has contraindication to or refuses radiation therapy, mastectomy is preferred.

What are the pros and cons for patients considering a mastectomy?
Many patients still prefer mastectomy because, naturally, they feel that it is safer for the entire affected breast tissue to be removed (even if only one area is diseased) and hence lower the risk of local recurrence when compared to lumpectomy. If done with immediate reconstruction, the appearance can look almost the same as her normal breast before the operation.
There are specific complications depending on the type of reconstruction used and patients are encouraged to discuss and make an informed decision. Nonetheless, I would like to stress that studies have shown comparable results in terms of survival between the 2 treatment modalities—mastectomy vs. lumpectomy and radiation therapy. Because of this, these two modalities are currently the gold standard for the surgical treatment of breast cancer.
The other thing to note is that most patients who undergo lumpectomy and sentinel lymph node biopsy recover more quickly than patients who receive mastectomy and major reconstruction (referring to as ‘flap reconstruction’). Lumpectomy can be done as a day surgery procedure as well, and the patient can be discharged home the same day.
Are there any new alternatives to the above procedures?
Yes. Cryoablation is a relatively new treatment modality for early breast cancer. So far, short-term studies (averaging 3-10 years follow up) have shown short-term effectiveness with comparable local recurrence rate to lumpectomy. Long-term effectiveness is still being evaluated and therefore, this treatment is still considered non-standard therapy.
Can you tell us more about the technology behind cryoablation and how it works? What studies have been done to show its effectiveness?
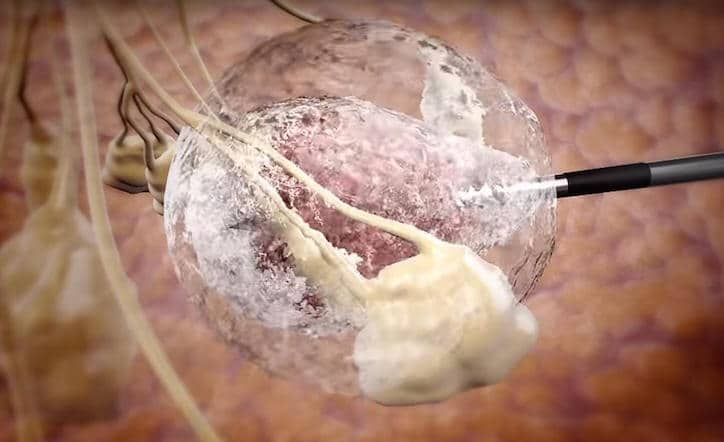
Cryoablation uses extreme cold temperature that flows through the specialised needle, called the cryoprobe, to cause deep-freezing and destruction of the tumour by way of ice formation. No living tissue, normal or diseased, can survive such extreme temperature (-170 degree Celsius).
A single institution study in Japan has been doing this for a selected group of early breast cancer patients for over 10 years, and has shown effectiveness in achieving local control comparable to that of lumpectomy. A multicentre trial in the USA called the ICE3 trial is ongoing and has finished their recruitment process. Last December, they reported their short-term data of 3 year follow-up with similar results. More studies are ongoing in Europe and Hong Kong, exploring the use of cryoablation on other more aggressive types of breast cancer and we are awaiting longer-term data, too.
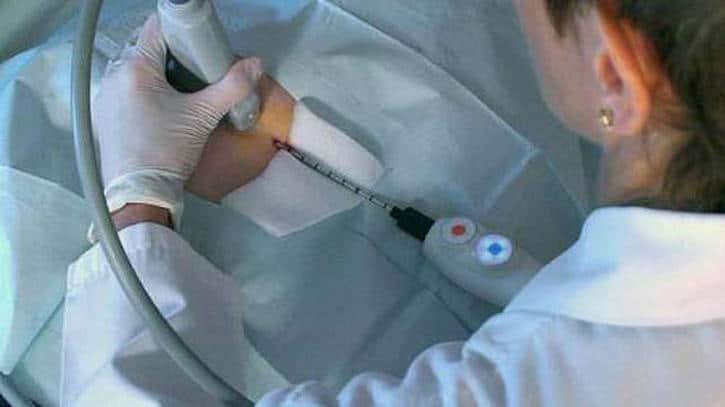
After anesthesia is given, the process of cryoablation begins with a small 5 mm skin incision, similar to when a person undergoes breast biopsy. This incision allows the placement of the cryoprobe. The actual cryoablation procedure used in the treatment of early breast cancer involves the “freeze-thaw-freeze” cycle and lasts about 30 minutes. At the end of the procedure, the cryoprobe is removed and the wound is closed. If the patient needs sentinel lymph node biopsy as well, that is done at the same sitting.
How cryoablation works in killing the cancer cells is 3-fold:
- The cancer cells in immediate contact with the cryoprobe are mechanically disrupted by the formation of ice crystals that form rapidly when the probe cools during the ‘freeze’ cycle. The cells not in contact with the cryoprobe become dehydrated during the process.
- In the Thaw cycle, fluids rushes back into the cell that became dehydrated during the freeze cycle. This rapid expansion of the cells cause it to burst and the cell membrane is further disrupted.
- During the freeze cycle, not only are tissue cells affected. Blood vessels nearby also become clotted, thereby depriving the cancer cells of blood flow and oxygen.
The end result of the “freeze-thaw-freeze” cycle is an area of dead tissue left within the treated breast. This can feel like a hard ball for the patient, and the body removes it over time. Researchers also believe that because the cancer cells are left dead inside the breast for our own body to clear, our immune system would be able to recognize the antigen that are presented on the cancer cells and may act as ‘auto-vaccine’ against recurrence of that cancer, because our immune system would have now recognized these as foreign. However, further data awaits on the confirmation of this effect.
Does cryoablation work in tandem with chemotherapy or radiation, or in place of them?
Cryoablation is meant to be used in place of lumpectomy. As breast cancer treatment is multimodal, a person deemed suitable for cryoablation must also receive radiation therapy, just like a person undergoing lumpectomy. Chemotherapy is recommended based on other tumour parameters and overall staging. Cryoablation does not replace chemotherapy. Researchers have found the effectiveness of combining cryoablation with drug therapy in some studies. The idea behind this is that cryoablation is used to break up the cancer cells, making them more exposed to the effects of drugs.
What are the side effects of cryoablation, and how do these compare to other treatments?
So far, there has been no reported adverse effects of cryoablation for the treatment of early breast cancer. This procedure can be performed as a day surgery procedure, with patients either fully awake and only under local anesthetics or with moderate sedation. The treatment time is usually approximately 30 minutes and the patient goes home afterwards. If the patient is fully awake during the procedure, they will experience coolness during the procedure. The skin is potentially at risk of severe thermal injury but there are measures put in place to prevent that, and there has not been a single case of skin necrosis reported. The breast will be slightly swollen at the end of the procedure and the patient can feel a hard ball in the area of treatment because of the dead tissue left inside (as explained above).
In my experience with cryoablation, patient satisfaction is high and recovery is quick. They report feeling normal the next day.
Cryoablation is also being investigated for use in other areas relating to breast cancer treatment, such as the use to freeze tumour metastasis to the bone. It has been reported by a European group that patients with bone metastases treated with cryoablation reported immediate relief of pain and in some cases do not require pain medications subsequently. This greatly improves their quality of life.
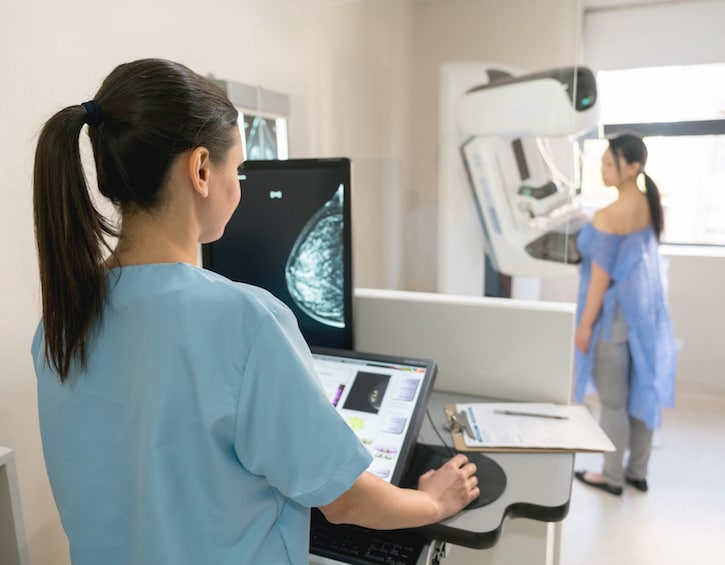
In recent years, there seems to have been some rethinking about the conventional wisdom surrounding mammograms and how frequently women should get them. Have any technological advances been made in terms of screening for breast cancer, or do you foresee anything on the horizon?
Screening recommendations vary from country to country and are subject to expert reviews and policy makers.
In recent years, tomosynthesis (aka 3D mammography) has become an important modality in the evaluation of breast diseases and in some countries or situations, it has been used as the primary screening and diagnostic modality. Tomosynthesis is useful for the evaluation of abnormality in dense breasts and has been shown to increase cancer detection rate. Furthermore it is available in Singapore. For high-risk cases, MRI remains the recommended modality.
Thank you, Dr. Jendana! If you’d like to speak with Dr. Jendana and get further information on breast cancer treatment options, you can contact her or visit one of PanAsia Surgery’s three clinics across Singapore.






 View All
View All




 View All
View All








 View All
View All








