
There seem to be a never-ending array of infections we need to be on the lookout for once the kiddos go off to school. But there are some bacteria that even babies are at particular risk for. Our microbiology expert Ellen Loveday weighs in on the risk factors and symptoms of the stubborn (and scary sounding!) MRSA bacteria.
As soon as someone says “MRSA” the first reaction for most of us is shock—we might even take a step away from the infected person!
Hospital patients, children, elderly home residents and some athletes are all at particular risk of developing a MRSA infection or “Super Bug”. This is because they generally are immune deficient or are in crowded environments.
So, is MRSA a fearsome disease that warrants jumping back in horror? Is it a normal part of life? To be truthful, the answer lies somewhere in the middle, but with proper diagnosis and treatment everything should eventually turn out OK.
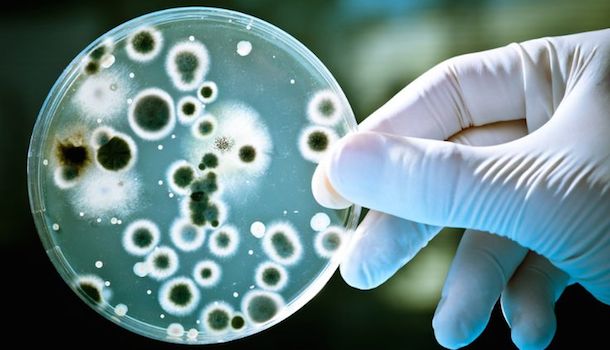
Medical facts
MRSA (Methicillim Resistant Staphylococcus aureus) is a bacteria that has mutated to become resistant to standard antibiotics, particularly Methicillin (from the Penicillin antibiotic family). Staphylococcus aureus grows in the nasal cavity of 25-30% of the population. About 2% of Staphylococcus aureus cases are MRSA.
The Center for Disease Control (CDC) considers the 5 C’s factors when discussing MRSA:
Crowded environments encourage spreading. Skin to skin contact is the number one method of spreading. Compromised skin (Cuts, cracks, eczema) is the most susceptible. Contamination occurs on surfaces through contact with an infected person. And lastly lack of cleanliness (i.e: washing of hands) is also a contributing factor.
MRSA appears like a boil, and often weeps as a clear yellowish liquid. Most infections are not life threatening. However, if the infection burrows deep into the skin, or is located in the bone, lungs or in joints, surgery may be needed to drain and treat the infection.

The best way to treat MRSA is to treat the patient with an antibiotic that is not from the Penicillin grouping for 7-10 days (such as oral antibiotics like Vancomycin, or for topical treatment, Bactroban ointment works well). Make sure that the patient completes the whole dose of antibiotics. This ensures that the bacteria does not survive and develop an additional antibiotic resistance.
The patient should avoid contact with others unless the infected site is covered. Surfaces and anything that the patient has come into contact with should be disinfected. Clothes and linen should be washed with detergent (separate from other laundry) and should be dried in a clothes dryer (NOT air-dried).
There is no need to close childcare or education facilities. Instead it is best to minimise the impact to others via clean hygiene routines of regular washing of surfaces with an antibacterial wash such as diluted Clorox.

Kids and Babies
Children in particular may have an area of their body that is susceptible to bacterial infections, such as under the chin of a teething baby. If the area is damp for most of the time, and it is warm and nutrient-rich, this creates a perfect breeding ground for bacteria. The best advice is to keep the area cool, dry and clean. Try using a zinc oxide cream to prevent the bacteria growth.
Once again, the best prevention is to avoid person-person contact with an open-wounded infected person, and continue to practice good hand washing techniques at all times.
Lead image sourced via Shutterstock, Image #1 sourced via Pinterest, Image #2 sourced via Shutterstock, Image #3 sourced via Shutterstock
References
CDC, 2013. Methicillin-resistant Staphylococcus aureus (MRSA) Infections. Centres for Disease Control and Prevention. Internet Site. Last viewed 11/12/2014. Available: www.cdc.gov/mrsa/
Mayo Clinic Staff, 2014. Diseases and Conditions MRSA Infections. Mayo Foundation for Medical Education & Research. Internet Site. Last viewed 14/12/2014. Available: www.mayoclinic.org/diseases-conditions/mrsa/basics/definition/con-20024479
WebMD, 2014. Understanding MRSA Infection – the basics. WebMD LCC. Internet Site. Last viewed 12/12/2014. Available: www.webmd.com/skin-problems-and-treatments/understanding-mrsa-methicillin-resistant-staphylococcus-aureus?page=2






 View All
View All





 View All
View All










 View All
View All




![[𝗛𝗢𝗧 𝗡𝗘𝗪𝗦] 𝗦𝗲𝗻𝗴𝗸𝗮𝗻𝗴 𝗦𝘄𝗶𝗺𝗺𝗶𝗻𝗴 𝗖𝗼𝗺𝗽𝗹𝗲𝘅 𝗶𝘀 𝗕𝗔𝗖𝗞 𝘄𝗶𝘁𝗵 𝗡𝗘𝗪 𝗦𝗟𝗜𝗗𝗘𝗦 & 𝗙𝗘𝗔𝗧𝗨𝗥𝗘𝗦! 💦🔥
One of the most popular pools in the North-East is finally back and it’s even better than before! Brand-new slides for thrill-seekers (1.2m+), splash zones for little ones, a Jacuzzi, sheltered teaching pool, and an Olympic-sized pool for serious swimmers.
Say goodbye to the rainbow slides as the new ones are faster, wider & way more fun! Just remember: proper swimwear only, and no accessories for max sliding speed.
𝗪𝗵𝗲𝗿𝗲: 57 Anchorvale Rd, Singapore 544964 (5 mins from Sengkang LRT)
𝗪𝗵𝗲𝗻: Tues/Thurs/Sat: 6.30am – 9.30pm | Wed/Fri/Sun: 8am – 9.30pm | Mon: Closed
𝗛𝗼𝘄 𝗺𝘂𝗰𝗵: Family of 4 (weekend) = Just $7!
Tag your splash squad & get ready for a wave of fun! 🏄♂️
.
.
.
.
.
.
.
#SengkangSwimmingComplex #SGPools #FamilyFunSG #WaterPlaySG #NorthEastLiving #SengkangReopens #KidsActivitiesSG #SengkangFun #publicswimmingpool](https://www.sassymamasg.com/wp-content/plugins/instagram-feed/img/placeholder.png)
